Diabetes is a chronic condition that affects millions of people worldwide, prompting many to seek effective treatments to manage their blood glucose levels. Among the numerous pharmaceutical options available, Ozempic has garnered significant attention. While this medication has proven benefits, it’s essential to explore its use from a naturopathic perspective to understand how it fits into a holistic approach to diabetes management.
What is Ozempic?
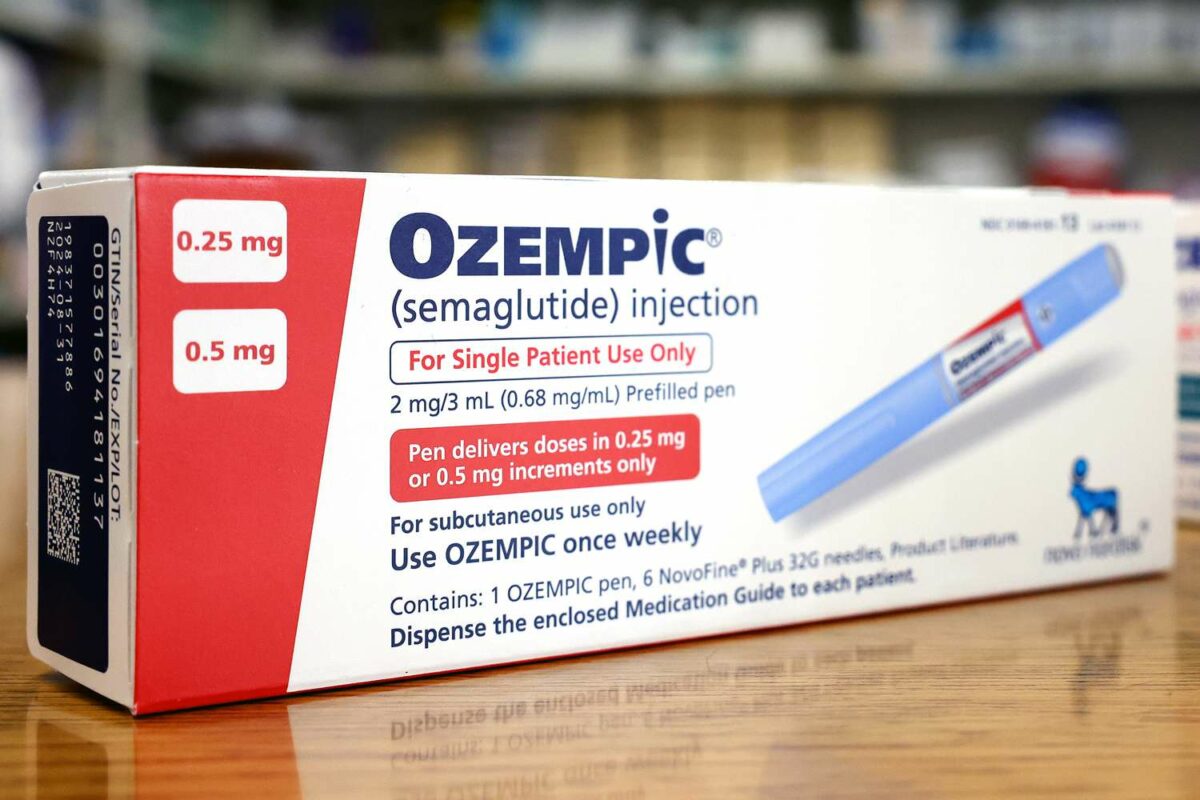
Ozempic is a brand name for semaglutide, a medication approved by the FDA for the treatment of type 2 diabetes. It belongs to a class of drugs called GLP-1 receptor agonists, which work by mimicking the incretin hormones that the body usually produces naturally to stimulate insulin secretion in response to meals. By enhancing insulin production, Ozempic helps to lower blood sugar levels effectively.
How Does Ozempic Work?
Ozempic works through several mechanisms:
- Stimulating Insulin Secretion: It enhances the release of insulin from the pancreas when blood sugar levels are elevated.
- Inhibiting Glucagon Release: It reduces the secretion of glucagon, a hormone that increases blood sugar levels.
- Slowing Gastric Emptying: It delays stomach emptying, which helps control post-meal blood sugar spikes.
- Promoting Satiety: It can help reduce appetite, which may lead to weight loss.
The Benefits of Ozempic
For many individuals with type 2 diabetes, Ozempic offers numerous benefits:
- Effective Blood Sugar Control: Clinical trials have demonstrated that Ozempic significantly lowers HbA1c levels.
- Weight Loss: Many patients experience weight loss while taking Ozempic, which is beneficial for those with type 2 diabetes.
- Cardiovascular Benefits: Some studies suggest that Ozempic may reduce the risk of major cardiovascular events in people with type 2 diabetes.
Naturopathic Principles and Diabetes Management
Naturopathy emphasizes the body’s innate ability to heal itself through natural means. This holistic approach to health focuses on treating the root cause of diseases rather than just the symptoms. Naturopathic treatments often include lifestyle modifications, dietary changes, herbal remedies, and stress management techniques.

Combining Ozempic with Naturopathic Methods
While Ozempic offers significant benefits, integrating it with naturopathic principles can lead to a more comprehensive diabetes management plan. Here’s how:
1. Diet and Nutrition
- Low Glycemic Diet: Incorporating foods with a low glycemic index can help stabilize blood sugar levels. Focus on whole grains, vegetables, lean proteins, and healthy fats.
- Anti-inflammatory Foods: Foods rich in omega-3 fatty acids, such as fish, flaxseeds, and walnuts, can help reduce inflammation, which is often elevated in individuals with diabetes.
- Herbal Supplements: Herbs like cinnamon, fenugreek, and berberine have shown potential in managing blood sugar levels. Always consult with a healthcare provider before adding supplements to your routine.
2. Physical Activity
- Regular Exercise: Engaging in regular physical activity, such as walking, swimming, or yoga, can improve insulin sensitivity and overall metabolic health.
- Strength Training: Incorporating strength training exercises can help build muscle mass, which in turn improves glucose uptake by cells.
3. Stress Management
- Mindfulness and Meditation: Practices like mindfulness meditation, deep breathing exercises, and progressive muscle relaxation can help reduce stress levels, which can positively impact blood sugar control.
- Adequate Sleep: Ensuring sufficient and quality sleep is crucial, as poor sleep can negatively affect insulin sensitivity and glucose metabolism.
4. Regular Monitoring and Consultation
- Blood Sugar Monitoring: Regularly monitoring blood sugar levels can help individuals understand how their lifestyle choices and medications affect their diabetes management.
- Consultation with Healthcare Providers: Working closely with both conventional healthcare providers and naturopathic practitioners can create a balanced and personalized treatment plan.

The Role of Naturopathy in Enhancing the Efficacy of Ozempic
By incorporating naturopathic practices, individuals can enhance the efficacy of Ozempic and achieve better overall health outcomes. A holistic approach ensures that all aspects of health—physical, emotional, and mental—are addressed, providing a more comprehensive treatment for diabetes.
Potential Synergies
- Improved Insulin Sensitivity: Lifestyle changes such as diet and exercise can improve insulin sensitivity, potentially reducing the dosage of Ozempic needed over time.
- Weight Management: Combining Ozempic with a healthy diet and regular exercise can enhance weight loss efforts, further improving diabetes management.
- Enhanced Well-being: Addressing stress and mental health can lead to better overall well-being, which is crucial for long-term disease management.
Potential dangers of Ozempic; can Naturopathy help?
Common side effects of Ozempic include gastrointestinal issues like nausea, vomiting, and diarrhea. Additionally, there are concerns about more severe complications such as pancreatitis, kidney problems, and thyroid tumours.
To offset some of these adverse effects, naturopathic medicine offers alternative and complementary approaches. For instance, incorporating herbal remedies like ginger and peppermint can help soothe digestive discomfort, while dietary adjustments rich in anti-inflammatory foods can support overall well-being. Supplements such as probiotics may also aid in maintaining gut health. By integrating these naturopathic strategies, individuals on Ozempic can potentially mitigate some of the drug’s side effects, promoting a more balanced and holistic approach to their health management.
Conclusion
Ozempic represents a powerful tool in the management of type 2 diabetes, offering significant benefits in terms of blood sugar control and weight loss. However, adopting a naturopathic perspective can provide a more holistic approach, addressing the root causes of diabetes and promoting overall health and well-being.
By integrating Ozempic with naturopathic principles, individuals can create a balanced and comprehensive diabetes management plan. This fusion of conventional and natural medicine can lead to improved outcomes, providing a path toward healthier living for those managing type 2 diabetes.
—
If you’re looking to explore a holistic approach to diabetes management, consider consulting with a naturopathic practitioner. They can provide personalized guidance and support, helping you integrate natural therapies with conventional treatments like Ozempic.
Your journey to better health starts today. Embrace the possibilities of a balanced approach and take control of your diabetes management with confidence.