Introduction to Glutathione
Ever heard of glutathione? It might be your body’s best-kept secret for optimal health. Glutathione is a powerful antioxidant produced in cells, composed largely of three amino acids—glutamine, glycine, and cysteine. It plays a crucial role in neutralizing free radicals, boosting the immune system, and detoxifying the liver. While our bodies naturally produce glutathione, factors like poor diet, pollution, toxins, stress, and aging can deplete its levels.
You can replenish glutathione through diet and supplements, but one increasingly popular method is glutathione infusion. This blog will explore why glutathione infusions are rapidly gaining attention among health enthusiasts, wellness seekers, and the aging population.
The Science Behind Glutathione Infusion
Why Bioavailability Matters
When it comes to supplements, bioavailability is key. This term refers to the proportion of a nutrient absorbed and utilized by the body. Oral glutathione supplements often suffer from low bioavailability due to the digestive process breaking down the compound before it can be absorbed. This is where glutathione infusion shines.
Intravenous vs. Oral Administration
Intravenous (IV) administration of glutathione bypasses the digestive system, delivering the antioxidant directly into the bloodstream. This method ensures nearly 100% bioavailability, allowing your cells to absorb the full dose. The immediate availability of glutathione helps cells to quickly combat oxidative stress and support various bodily functions.
Cellular Impact
At a cellular level, glutathione acts as a detoxifier, removing harmful substances from cells. It also regenerates other antioxidants like vitamins C and E, further contributing to cellular health and longevity. This makes glutathione infusion a potent tool for enhancing cellular function and overall wellness.
Uses and Benefits of Glutathione Infusion
Detoxification
One of the primary roles of glutathione is detoxification. It binds to toxins, heavy metals, and carcinogens, making them water-soluble and easier for the body to excrete. For those exposed to high levels of environmental toxins or undergoing detox programs, glutathione infusion can be a game-changer.
Immune System Support
A robust immune system is essential for maintaining health. Glutathione is vital in regulating the immune response, promoting the proliferation of white blood cells, and enhancing their activity. By boosting glutathione levels through infusion, you can support your immune system in fighting infections and diseases more effectively.
Anti-Aging Effects
The anti-aging benefits of glutathione are hard to overlook. This powerful antioxidant reduces oxidative stress, a key factor in aging. By neutralizing free radicals, glutathione helps to slow down the aging process, reducing the appearance of wrinkles and fine lines. It also supports the repair and regeneration of tissues, contributing to youthful, glowing skin.
Skin Health
Glutathione is often dubbed the ‘master antioxidant’ for skin health. Its ability to lighten and brighten the skin by inhibiting melanin production makes it a popular choice for those seeking a more even complexion. Regular infusions can help reduce hyperpigmentation, age spots, and acne scars, giving you a clearer, more radiant skin tone.
Who Can Benefit from Glutathione Infusion
Health Enthusiasts
If you’re someone who’s always looking for ways to optimize your health, glutathione infusion could be a valuable addition to your wellness routine. Its detoxification and immune-boosting properties can help keep your body in peak condition.
Wellness Seekers
For those on a continuous quest for wellness, the holistic benefits of glutathione infusion make it a compelling option. Whether you’re dealing with stress, fatigue, or simply want to improve your overall well-being, glutathione can support your wellness goals.
Aging Population
Aging brings about a host of challenges, from decreased immune function to increased oxidative stress. Glutathione infusion offers a natural way to combat these issues, promoting longevity and a better quality of life as you age.
Specific Health Conditions
Individuals with certain health conditions, such as chronic fatigue syndrome, autoimmune diseases, and liver disease, may find glutathione infusion particularly beneficial. Its powerful antioxidant properties can help manage symptoms and improve overall health outcomes.
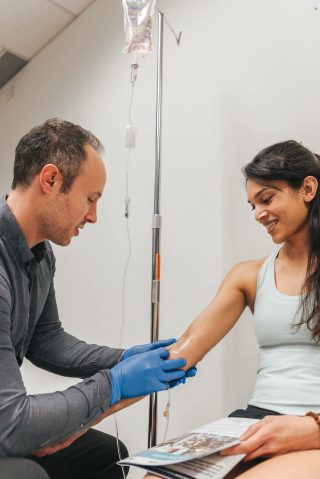
The Process of Glutathione Infusion
What to Expect
Curious about what happens during a glutathione infusion session? Typically, the process is straightforward and takes about 30-60 minutes. A healthcare professional like myself will administer the glutathione solution intravenously, ensuring it enters your bloodstream directly.
Duration and Frequency
The duration of each session varies, but most people spend about 45min receiving the infusion. Depending on your health goals and the advice of your healthcare provider, you might need multiple sessions over several weeks or months.
Potential Side Effects
While glutathione infusion is generally considered safe, some people may experience minor side effects like discomfort at the injection site or mild headaches. It’s essential to consult with a healthcare professional to determine if this treatment is right for you.

Glutathione and Lifestyle
Dietary Sources
While infusions are highly effective, it’s also important to support your glutathione levels through diet. Foods rich in sulphur, such as garlic, onions, and cruciferous vegetables, can boost glutathione production. Additionally, consuming foods high in antioxidants, like berries and nuts, can further support your body’s antioxidant defences.
The Role of Exercise
Regular physical activity has been shown to increase glutathione levels in the body. Incorporating exercises like weight training and cardiovascular workouts into your routine can help maintain optimal glutathione levels and overall health.
Holistic Approach
A holistic approach to health and wellness doesn’t rely on one single treatment. Combining glutathione infusion with a balanced diet, regular exercise, and stress management techniques can maximize your overall well-being.
Conclusion and Next Steps
In summary, glutathione infusion offers a myriad of benefits, from detoxification and immune support to anti-aging and improved skin health. Whether you’re a health enthusiast, a wellness seeker, or part of the aging population, this powerful antioxidant can significantly enhance your quality of life.
If you’re interested in exploring glutathione infusion further, consider booking a consultation. For additional resources, check out our recommended reading list and expert blogs on this topic.
Ready to experience the benefits of glutathione infusion for yourself? Start your journey to better health today!
Reading List:
https://www.medicalnewstoday.com/articles/323936
Tanzilli G, Arrivi A, Placanica A, Viceconte N, Cammisotto V, Nocella C, Barillà F, Torromeo C, Pucci G, Acconcia MC, Granatelli A, Basili S, Dominici M, Gaudio C, Carnevale R, Mangieri E. Glutathione Infusion Before and 3 Days After Primary Angioplasty Blunts Ongoing NOX2-Mediated Inflammatory Response. J Am Heart Assoc. 2021 Sep 21;10(18):e020560. doi: 10.1161/JAHA.120.020560. Epub 2021 Sep 17. PMID: 34533039; PMCID: PMC8649545.
Arrivi A, Pucci G, Placanica A, Bier N, Sordi M, Dominici M, Carnevale R, Tanzilli G, Mangieri E. Early and prolonged glutathione infusion favorably impacts length of hospital stay in ST-elevation myocardial infarction patients: a subanalysis of the GSH2014 Trial. Minerva Cardiol Angiol. 2023 Apr;71(2):147-152. doi: 10.23736/S2724-5683.22.06134-8. Epub 2022 Sep 9. PMID: 36083043.